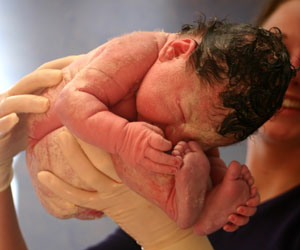
The term “baby catcher” refers to the humble philosophy of midwives that it is the mother who actually delivers her baby, and her midwife is simply there to catch it.
And I’ll be the first to admit, when I first heard the word “midwife,” it brought to mind an image of a woman with a little black bag approaching a cabin in the backwoods to catch a baby.
But that’s not the reality: “Midwife” means “with woman.” The United Nations’ World Health Organization (WHO) defines a midwife as one who “must be able to give the necessary supervision, care, and advice to women during pregnancy, labor, and the postpartum period and conduct deliveries on her own responsibility.”
Fast forward a few years, and now when I tell strangers that I gave birth naturally with the assistance of a midwife—yes, that’s right, no epidural—I sometimes catch them off guard. “Really? Wasn’t it painful?” Well, sure, a little, but I wouldn’t have changed a thing. A cab driver sped through Manhattan to get me to the birthing center, where my daughter was born just two hours after I arrived. My midwife was a super-coach who let me walk around the room, soak in a whirlpool, and sway to the music I’d brought. Nothing unusual there, right?
Still, in our country, engaging the services of a midwife instead of a doctor is not the norm. “The latest figures show that 10 percent of all births in this country now are attended by midwives, rather than doctors,” says Marsden Wagner, M.D., M.S., an independent maternity care consultant and former director of Women’s and Children’s Health for WHO. Although this figure might sound low, it’s actually a “very significant increase” in American healthcare, according to Wagner. Still, it is a small number when compared to, say, Europe, where midwives attend 75 percent of all births.
Tough trade with many rewards
“It’s not a great climate for the kind of midwifery that I used to practice,” says Peggy Vincent, a Certified Nurse Midwife from Berkeley, CA, who “caught” well over 2,500 babies during her more than two decades as a midwife. Across the country, midwives agree that it’s challenging to exist in the modern world, especially when it comes to things like acquiring insurance and educating the public about the competency of midwives. In fact, while writing this article, I discovered that the practice I’d used—Midwifery Services, the first autonomous midwifery practice in the United States, which started in 1974—closed its doors just last year.
Geradine Simkins, vice president of Lilburn, GA-based Midwives Alliance of North America (MANA), says midwifery burgeoned  during the late 1960s and 1970s: “Women not only began to question the dominant medical model of maternity care in the United States, but they also began to demand a more woman-centered, family-focused natural model of childbirth.” So, what’s the difference between midwives and doctors? In Vincent’s opinion, midwives believe that birth is normal until proven otherwise and doctors do not. In other words, Vincent says that doctors sometimes “assume that a lot can go wrong, so they are continually testing and looking” for medical problems that need to be solved with extraneous or invasive procedures. Whereas midwives “operate under the belief that women’s bodies were intended to have babies” and therefore their methods are based on allowing for natural facilitators to the process of giving birth.
during the late 1960s and 1970s: “Women not only began to question the dominant medical model of maternity care in the United States, but they also began to demand a more woman-centered, family-focused natural model of childbirth.” So, what’s the difference between midwives and doctors? In Vincent’s opinion, midwives believe that birth is normal until proven otherwise and doctors do not. In other words, Vincent says that doctors sometimes “assume that a lot can go wrong, so they are continually testing and looking” for medical problems that need to be solved with extraneous or invasive procedures. Whereas midwives “operate under the belief that women’s bodies were intended to have babies” and therefore their methods are based on allowing for natural facilitators to the process of giving birth.
There are many kinds of midwives, but they can generally be classified into one of two categories: According to MANA, a direct-entry midwife “is an independent practitioner educated in the discipline of midwifery through self-study, apprenticeship, a midwifery school, or a college- or university-based program distinct from the discipline of nursing.” A direct-entry midwife primarily works in out-of-hospital settings. And a nurse-midwife is one who has been educated in the two disciplines of nursing and midwifery and is certified according to the requirements of the American College of Nurse-Midwives. This type is most often found catching babies in a hospital setting.
From western medicine to midwifery
“I’m probably one of the few midwives who didn’t dream of being a midwife,” says Vincent, who caught her last baby in 2006 before she retired. Instead, Vincent started her career in the late 1970s as a staff nurse at Alta Bates Hospital in Berkeley, CA, where she had “a very cushy position”—a day shift with full benefits. In her memoir, Baby Catcher: Chronicles of a Modern Midwife, Vincent recalls that she had never paid much attention to the local “lay,” or unlicensed, midwives, because in those days they were considered “a shadowy presence lurking on the fringe of organized medicine. They were deliberately under-cover, because they were afraid of getting in trouble,” Vincent says. In fact, she never considered searching out a midwife for the birth of her first child. But when she came very close to delivering her second child at home, Vincent began keeping her eyes out for “these mystery women.”
She met her first midwife in 1974, when a labor dispute at Alta Bates left the hospital very short-staffed. Carole Hagin, a highly respected local lay midwife and mother of seven children, was invited in to relieve some of the nurses. After watching Hagin calmly talk women through labor, rather than hooking them up to IVs, Vincent was eager to change careers despite the challenges. “I knew that if I left and became a midwife, I’d have no health insurance,” she recalls. “But it was either become a bitter nurse or become a midwife.” So she enrolled in San Francisco General Hospital’s midwifery program, the same place where Hagin had studied. In her class of 12, she was one of only a few students who came from western medicine rather than lay midwifery.
Dealing with doctors
Vincent’s ability to cross over probably worked to her great advantage when she founded the Alta Bates’ birthing center in 1977. “I went from medicine to midwifery, so I felt like I could travel between both worlds,” she says. “You have to know how to talk to doctors—that was easy for me. I also had the support of the entire nursing staff at Alta Bates; they were solidly behind me.”
Lisa Coomer, a Certified Professional Midwife in Knoxville, TN, agrees that the line between the medical establishment and midwifery can be a tricky one. “In Knoxville, years ago, they were not very accepting of midwives in hospitals,” says Coomer, who became a direct-entry midwife in 1986, “when there were only six states where you could legally work.” Interviewed for this article just hours after delivering a baby girl at home, Coomer recounts: “It was so beautiful to watch this woman who’d had a hospital birth with her first baby,” she says. “The mother was smiling at me as her baby was crowning. I had her reach down and take the baby. It still astounds me!”
Coomer, who has caught more than 500 babies over the past two decades, followed a similar path to Vincent’s when, after having her first child in a hospital, she decided on a home birth for her second baby. After Coomer’s 10.5-pound daughter entered the world at home, she remembered, “I wanted to get on the roof and yell out to women how great this can be.” Inspired, she signed up for midwifery school and found her new goal in life: to help women giving birth “to see what they’re capable of,” Coomer adds. “I’m so honored to be doing this.”
Midwife matchmaker
If you’re pregnant and interested in finding a baby catcher, it’s important to be informed. Follow these tips to decide if a prospective midwife can meet your needs and provide the care you seek.
First, Coomer suggests asking a midwife how she was certified and whether she’s licensed by her state. Also make sure that she has a doctor she refers to, or get your own doctor on board as a backup and ensure the doctor is supportive of your decisions. Coomer also recommends asking for references of other mothers and doctors the midwife has worked with in the past.
Elizabeth Moore, a Certified Professional Midwife in Boulder, CO, who practices outside of the hospital setting, offers women a free, one-hour meeting in which “you can really ask all of your questions in a nice meet-and-greet.”
All the midwives interviewed agree that after you get the facts, it’s really a gut decision about whether you click with a particular midwife. “Obviously, you want to know if your midwife has a good reputation as well as experience,” says Moore, who is also public education project manager at MANA. “But I think the decision comes from a much deeper place, such as, are you comfortable with this woman?”
There’s no doubt that midwives are passionate about what they do. When asked what drives her in a profession that can be challenging in today’s modern world, Moore says, simply, “for women to understand the joys of birth, this is the most affirming life can get.”
— Rachel Sarah



Leave a Reply